Periodontitis

‘Hopeless’ teeth because of periodontitis? No!
Being able to bite into a fresh apple is a visible sign that you’ve got good oral health and stable teeth. But even if your teeth are compromised by gum disease, you and your dentist can work together to stop the infection in its tracks. Make your teeth strong again and restore your bright and healthy smile!
How does gum disease look like?
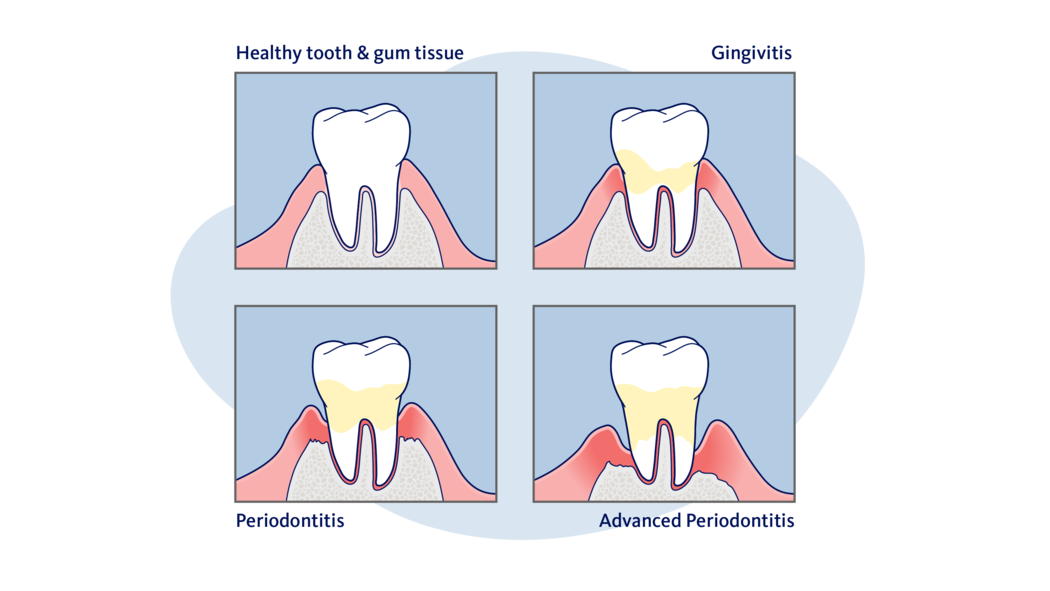
Periodontitis, often called gum disease, is caused by the body’s response to bacteria on the surface of the tooth, which is also known as dental plaque or bacterial biofilm. If you are experiencing reddened and swollen gum tissue (gingiva), or bleeding gums, this may be warning signs that you’re suffering from periodontal gum disease.
If not treated gum disease progresses into more severe diseases such as periodontitis. With gingivitis, only the gums are inflamed, but with periodontitis, the inflammation also extends to the bone underneath and includes bone loss or bone resorption.
This is often invisible and doesn’t cause any pain. But there are other symptoms of periodontitis you may experience, for example bad breath, and as time goes by, the teeth can become loose (mobile teeth) due to loss of supporting bone and may change their position.
In advanced periodontal disease, patients may lose a tooth or may need to have a mobile tooth extracted. This can be the case if the bone loss is too severe or if there are additional problems, such as a root canal infection or an infection in the tip of the tooth’s root.
Can periodontitis be cured?
With the right treatment, periodontitis can be stopped at any stage – not just in the early stages of gum disease (early periodontal disease). Even ‘hopeless’ teeth can be saved with the right surgical procedure, frequent follow-up appointments including professional cleaning and, of course, your cooperation – by quitting smoking and maintaining good oral hygiene, for example.
How does periodontal surgery work?
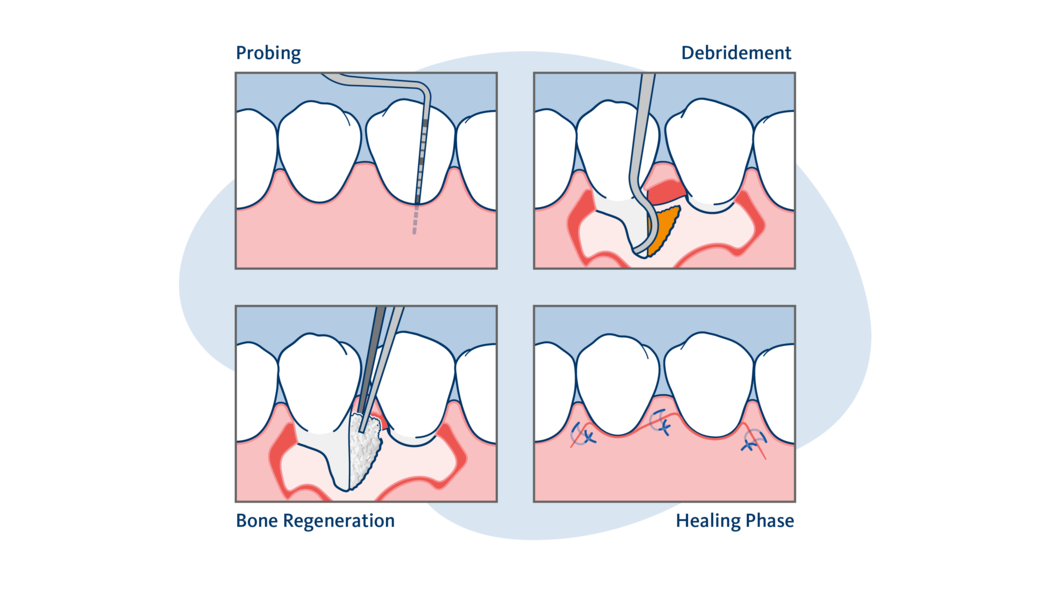
1 Examination: Your dentist will first thoroughly examine the condition of your teeth and gums. They will take into consideration whether your gums are swollen and inflamed, whether there is bleeding or pus when they insert a probe into the small gap between tooth and gums, and whether bone loss around your teeth is already visible on an X-ray. They will also discuss your individual risk factors such as smoking habits or health problems with you.
2 Cleaning the tooth’s root surface/deep cleaning: Treating periodontitis always starts with cleaning the tooth’s root surface using special tools. Your dentist or dental hygienist calls this deep scaling and root planing, and it involves scratching the bacterial biofilm off the roots without making any incisions in your gums. Some dentists use a periodontal curette, others use ultrasonic devices, and others use a combination.
If the gums are inflamed, they will appear swollen. By getting rid of the bacteria, this inflammation is stopped, and the gums can recover. Because of this process, the gum line may slightly change when the gums become healthy again.
3 Deeper cleaning/periodontal surgery: In some cases, non-surgical cleaning is insufficient. Then, the bacteria are too deep inside the periodontal pockets, and the dentist may not be able to reach them without making a small incision in the gums to give them a better view. This is known as surgical debridement or open flap debridement.
4 Creating new bone: Sometimes, dentists may add a bone substitute or other agents to help the bone grow back. This method gives you the chance to start over again with stable teeth surrounded by healthy bone and gums. Whether or not this regenerative approach is suitable for you depends on the kind of bone loss you’re experiencing, the shape of the defect and other factors.
5 Final Step - Esthetics: After successful periodontal treatment, the gum line can be corrected with gum graft surgery to improve the esthetics of your teeth and gums. Orthodontic treatment can also help, as it re-aligns the teeth in the correct position and can even help you to re-gain more of the lost bone volume.